Vitamin D: Mouse/Pet Killer or COVID-Fighter?
What everyone should know about testing Vitamin D levels in their blood
The optimal level of Vitamin D in the blood, and its role in fighting severe COVID-19 is a hotly debated topic which is also scientifically complex and confusing. Do we need Vitamin D supplements? Is too much Vitamin D toxic to us or our pets? Here is a summary of what we know, and don’t know1:
What is it?
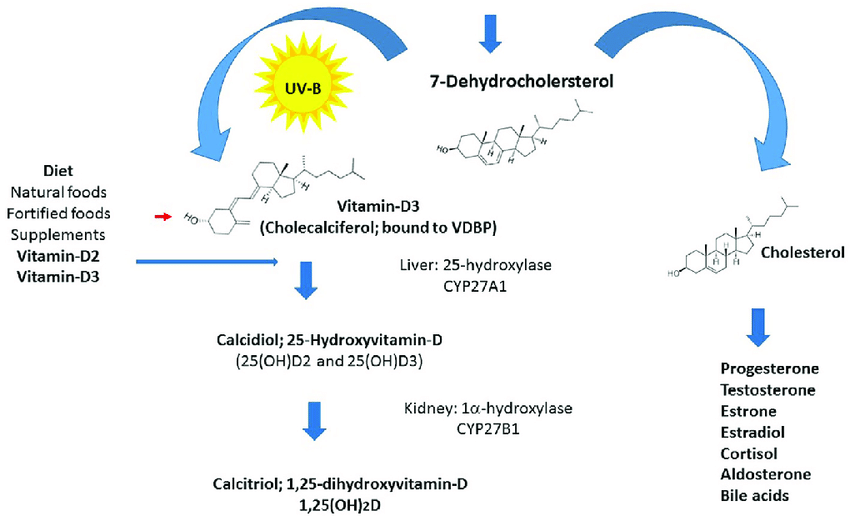
Our skin, when exposed to UVB rays from sunshine, converts a precursor of Vitamin D into Vitamin D. That is why individuals living at higher latitudes, in cities with polluted air, and/or with darker skin are likely to have lower levels of vitamin D. The cutaneous (skin-related) precursor to Vitamin D is also a precursor to cholesterol, which is by itself a precursor to many other hormones in the body such as testosterone. That is why some researchers now call Vitamin D another hormone in our body. Hormones are signaling molecules in our blood responsible for proper metabolism and homeostasis (balanced body functions) of our body.
The precursor plus dietary Vitamin D sources (like supplements or dairy products) feed liver with the Cholecalciferol (D3) form of the vitamin, which is converted to the Calcidiol (25-Hydroxy or 25(OH)), the form usually reported in clinical blood test results, which is then converted to Calcitriol2 or 1,25(OH)D2, which is the active form of Vitamin D responsible for absorbing calcium from food in our intestines into our blood.
Why does our body make Vitamin D in two steps, first an inactive form, then a bio-active form? Because if there is too much or too little calcium in the blood, the body can sense that and send a feedback signal to kidney to make less or more of the active Vitamin D form to stabilize calcium levels. Many other hormones are produced the same way in our body (for example T3 and T4 forms are part of the feedback loop of thyroid hormone). The body first makes an intermediate (precursor) form of the hormone and then a final active form depending on the needs of the body. I discuss such biological (homeostatic) feedback loops in my book.
What Does it Do?
Other than absorption of calcium into the blood from food in our intestines, Vitamin D is shown to play important physiological roles in our immune system (adaptive and innate), antimicrobial defense, the microbiome, and preventing neurological disorders such as multiple sclerosis (MS), schizophrenia and autism. For example, vitamin D is shown to inhibit the production of pro-inflammatory Th1 cytokines and stimulate the production of anti-inflammatory cytokines as well as regulatory T-cells (Treg).
Controversy over Optimal Plasma Levels
There is some controversy over the optimal level of Vitamin D in the blood. A number of studies suggest the optimal serum 25(OH)D concentration range for both skeletal (calcium metabolism into body and bones) and non-skeletal (immune and neurological) health is around 30-50 ng/mL. Because Vitamin D is fat soluble, studies have shown that overweight or obese individuals tend to have lower serum (blood) concentrations of vitamin D and may need more sunlight or supplementation than people with normal weight. But overweight individuals are also more prone to toxic overdosing on Vitamin D supplementation if their body doesn’t need it because excess Vitamin D is stored in fat cells (adipose tissue) in the body.
Does it Help with the Severity of COVID-19?
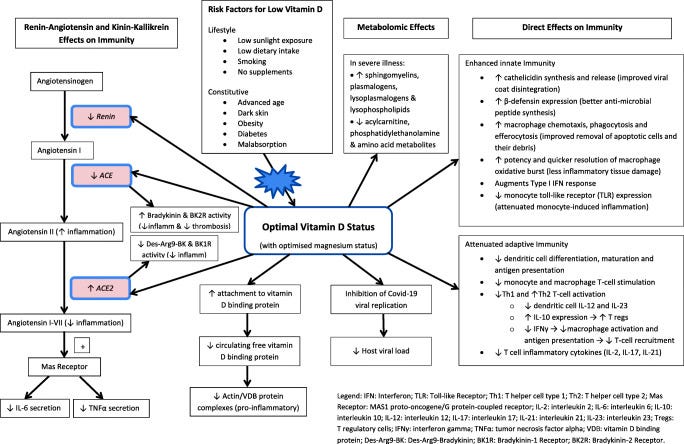
Meta-analysis of COVID-19 data from 19 countries has revealed that COVID-19 mortality sharply decreased in patients with plasma Vitamin D3 levels above 30 ng/mL. It is unclear if the low Vitamin D levels were a cause or an effect of the infection but the authors believe low Vitamin D 3 is a predictor rather than a side effect of infection3. In another study, Irish researchers from 10 research centers reviewed 270 studies from several countries to conclude: “There are now multiple evidential strands linking low vitamin D status to increased SARS-CoV-2 infection and COVID-19 disease severity… Data present compelling evidence for a protective effect of Vitamin D against COVID-19. We recommend that adults in Ireland should be supplemented with oral vitamin D3 at 20–25 μg/day (800–1000 IU/day) for the duration of this pandemic. For those who are overweight or obese, or who have dark skin pigmentation or other risk factors for vitamin D deficiency, it is likely that supplementation at daily doses higher than this will be required to achieve the serum 25(OH)D levels needed for optimal immunity.” This is how the authors visualize potential mechanisms of action by Vitamin D against COVID-19.
You can find good reviews of Vitamin D-related research papers on vitaminDforall.org by a group of doctors and scientists.
Low vitamin D levels are shown to be associated with low ionized calcium levels in COVID-19 patients. This is probably because calcium plays an important role (in coordination with magnesium, potassium, sodium and Vitamins K2 and D) in vasoconstriction (tightening of blood vessels) particularly in times of infectious injury, in coagulation, platelet adhesion, contractility of myocardial (heart) and smooth muscle cells. These are associated with the pathophysiology of COVID-19.
Is Too Much Supplementation Bad?
Too much Vitamin D in the human blood is called hypervitaminosis D, which could be toxic because Vitamin D pulls calcium along with it into the blood, and as we just noted, calcium mediates cellular functions such as blood clotting and blood pressure. Too much Vitamin D is sometimes defined as: (1) Clinical features of hypercalcemia (too much calcium in the blood, for example caused by an overactive parathyroid) such as kidney stones, (2) elevated serum calcium levels, (3) reduced or normal levels of serum parathyroid hormone (PTH), and (4) vitamin D levels of >100 ng/mL. However, according to the Institute of Medicine (IOM) guidelines patients with serum 25(OH)D levels of >50 ng/mL are at risk of toxicity.
Is it a Rodent Poison?
In smaller animals, Vitamin D can be lethal. In fact, some popular brand of pest control use Cholecalciferol (Vitamin D3) as mouse and rat poison. Most rodenticide baits contain 0.075% cholecalciferol. According to Merck Veterinary Manual “Cholecalciferol toxicosis is characterized by hyperphosphatemia and hypercalcemia (high blood levels of phosphorous and calcium), leading to renal failure, cardiac abnormalities, hypertension, CNS depression, anorexia, vomiting, diarrhea, and lethargy. The increased calcium and phosphorus can lead to calcification of soft tissue, notably the highly vascular areas of kidneys and lungs, as well as within the walls of the great blood vessels.” In rodents, the vasoconstriction and ossification of blood vessels, kidneys, lungs and heart muscles lead to hemorrhaging and death. Small doses of Vitamin D (less than 2000 IU) are usually not toxic to adult humans but may be toxic to children and pets.
Calcium Overload in the Blood
Although too much Vitamin D can lead to too much calcium in the blood but if the source of high calcium in the blood is an overactive parathyroid (hyperparathyrodism), Vitamin D supplementation can be used to treat the condition. So if your blood calcium levels are too high, before you can judge if you have too much or too little Vitamin D in your blood, you need to measure the parathyroid hormone in your blood too.
Seasonality and Weather Relations
Research in Lithuania shows that the lowest vitamin D status was found in December, January, February, March, and April. A study in India shows Vitamin D levels are even higher in the rainy season than in the summer. This could be caused by cleansing of air by rain from pollutants that block UVB rays.
These findings can explain the severity of Vitamin D deficiency (and COVID-19) in colder months in large polluted cities of the world with high levels of particulate matter and ozone in the air, such as New York, Milan and Tehran. In fact, the Lombardy region in northern Italy, which ranks among the most air polluted areas of Europe, was the hardest hit with COVID-19 and tracked as an epicenter of the outbreak. An ecological study shows air polluted with particulate matters in Lombardy, Italy was significantly associated with the COVID-19 incidence and excess mortality during the first wave of the outbreak.
Am I Deficient in Vitamin D?
The exact amount of Vitamin D we may need in supplements depends on many factors such as our exposure to sunshine and our area’s latitude and air pollution levels, our skin color tone, our body mass index and amount of adipose (fat) tissue, our plasma levels of potassium, sodium, calcium, phosphorous, magnesium and Vitamin K2 in the blood, as well as our neurological health and immune systems’ infectious load. You need to ask your doctor or lab to include Vitamin D biomarker in your blood test. Usually Calcidiol form 25(OH)D2 levels are tested and reported. But if you have problems with your kidneys (such as recurring kidney stones or other issues) or calcium metabolism (via parathyroid) your doctor may want to also test for the 1,25(OH)2D (Calcitriol) form released by kidneys. Elevated Calcitriol levels may be due to an overactive parathyroid and in fact a sign of Vitamin D deficiency and need for supplementation.
If your Vitamin D (25(OH)D2) levels are below the 30 ng/mL threshold (for adults), consider spending more time outdoors in the sun. Supplementation with 2000 IU per day of pure vitamin D may help especially in colder months and higher latitudes, and in people who have darker skin colors (absorb less UVB from sunshine), or those living in air-polluted cities or exposed to infectious diseases. If your blood calcium levels are not too high, you can also benefit from whole (not low fat or fat-free) milk which not only has Vitamin D but also balances it with calcium, phosphorous, Vitamins A and B, and Vitamin K (proper blood clotting and bone formation). Fresh local whole organic milk from pasture-raised cows are the best. Another potent naturally-balanced source of Vitamin D for adults is cod liver oil, which is pricey and hard-to-find in premium quality.
The information provided is for educational purposes only, and is not a substitute for professional advice.
‘Tri means 3, and ‘ol means OH group, because it has 3 hydroxyl groups.
Because Vitamin D3 is a negative renin-angiotensin system (RAS) modulator by inhibition of renin expression and stimulation of ACE2 expression. Vitamin D3 also decreases the production of pro-inflammatory Th1 cells.