These Factors Aggravate Disease with Coronavirus (Cold) and Flu Viruses: 35 Years of Research
Important research not shared by commercial mass media and most sponsored scientists
Did you know that a group of researchers have spent about 35 years to identify common factors that predict who among us becomes seriously ill when we are exposed to influenza or cold viruses (such as Coronavirus type 229E) affecting the upper respiratory tract?
According to research published in 1991, when people were given nasal drops containing one of five respiratory viruses (such as Coronavirus type 229E) not everyone developed a symptomatic cold. Incidence of symptomatic (clinical) disease among those infected ranged from 27% to 47%. The risk was found to be associated with ..
the level of chronic physical and psychological (perceived) stress, as described below.
Sheldon Cohen’s group has been working on the topic for decades. In a more recent publication, Cohen has found factors associated with greater risk of respiratory illnesses after virus exposure including smoking, ingesting an inadequate level of vitamin C, and chronic psychological stress. Factors associated with decreased risk included social integration, social support, physical activity, adequate and efficient sleep. Cohen cautiously suggests that his findings could have implications for identifying who becomes ill when exposed to severe acute respiratory syndrome Coronavirus 2 (SARS-CoV-2), the virus responsible for Coronavirus disease 2019 (COVID-19).
If Cohen is right, being isolated from friends and family may reduce the risk of viral exposure but it also weakens our immune system at the same time. Cohen’s research makes sense because we now know that our immune, neurological, and psychological systems are closely intertwined. That is why psychiatrist George Engel referred to humans as a Biopsychosocial species.
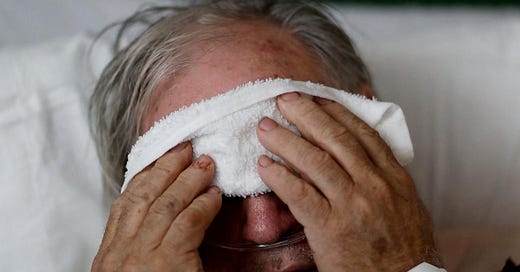
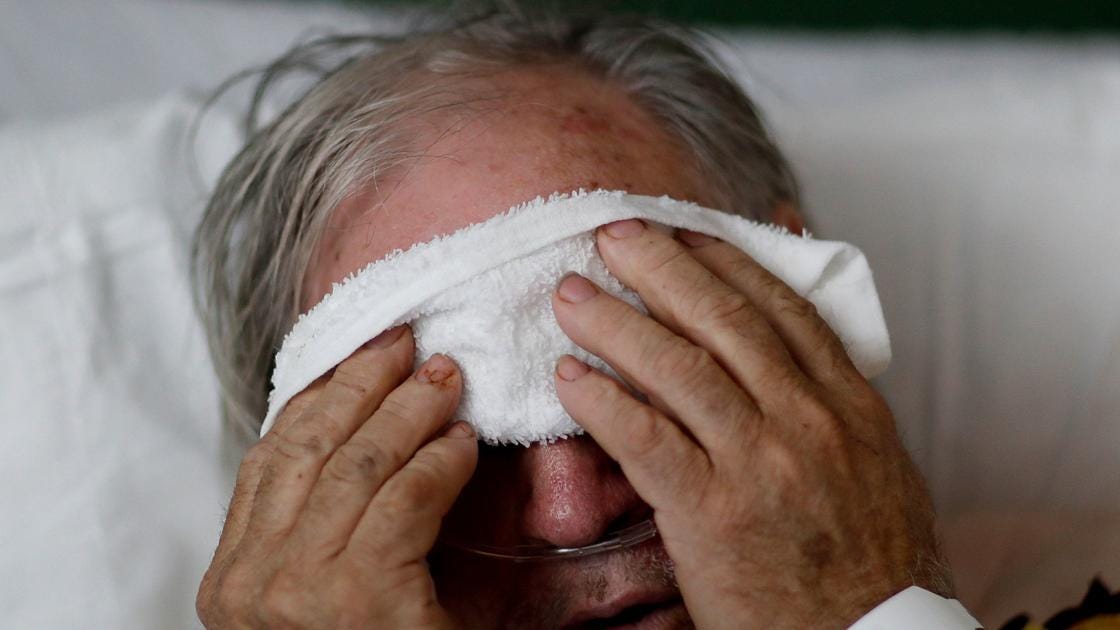
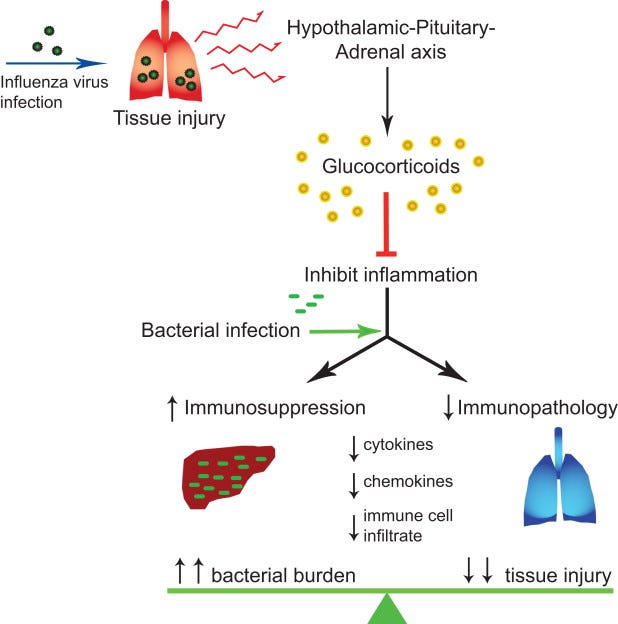
An important hormone that mediates both our body’s psychological and physical responses to stress and anxiety is cortisol. In my book (to be published early in 2022) I describe the many different roles of cortisol in our body, including a feedback loop that controls when our body stops (over)reacting to pathogens. For example, researchers have found that influenza infection triggers a sustained increase in serum glucocorticoid levels, which results in a systemic suppression of immune responses. Yet this virus-induced glucocorticoid production is necessary to control (balance) the inflammatory response and prevent lethal immunopathology during coinfection with viruses or bacteria (as seen in the image above).
Cohen, however, argues that
prolonged (perceived) stress alters the effectiveness of cortisol (stress hormone) to regulate our body’s inflammatory response because it decreases tissue sensitivity to the hormone. The scientific term for this is glucocorticoid receptor resistance. People who are regularly less able to regulate their inflammatory response, produce more of inflammation-inducing cytokines (chemical messengers) and suffer from more severe symptoms when exposed to viruses and pathogens. In fact, Italian researchers confirm a link between chronic excessive (stress-induced) glucocorticoid exposure and suppressed immune response to infective states, including possibly COVID-19.
Other research by Cohen has shown that chronic stress (and anxiety), lasting for a month or more, affected the risk of catching a cold. Two causes of stress – being unemployed or underemployed, or having interpersonal difficulties with relatives or friends – had the greatest influence on risk. Cohen has also reported that people with the most ties to relatives, friends and community were the least likely to catch a cold even though cold viruses spread more easily among connected clusters of people than among quarantined isolated individuals. Although this finding would seem counter-intuitive, Cohen asserts that “having many different kinds of social relationships helps to protect against disease.”
The punchline of all this science: While it’s important to look for medical treatments and vaccines to help people with weaker immune systems, we should not ignore the critical role of chronic stress in our vulnerability to infectious diseases. For many people, the stress of being isolated, fearful, anxious, inactive, quarantined, unemployed or underemployed, if prolonged, may weaken their immune system more than the viruses can!